
The U.S. Food and Drug Administration (FDA) considers tattoo ink to be a cosmetic. But what is really in the ink? Angie Seelal, PA-C explores this question.

Dermatologist Dr. Suzanne Friedler with Advanced Dermatology PC clarifies the symptoms and treatments for both Psoriasis and Eczema

Dermatology APRN Denise Gallo with SkinCare Physicians of Fairfield County, a division of Advanced Dermatology PC, with tips on understanding and treating warts

Dermatologist Cybele Fishman, MD, recommends her preferred products this holiday season.

Suzanne Friedler, M.D., a board-certified dermatologist who knows what ingredients to look for in a body wash and for the low-down on fragrance in skincare products.

Fungal acne isn’t even acne at all, to begin with. It was given the moniker of “fungal acne” because of its appearance. Get all the details from dermatologist Cybele Fishman, MD.

board-certified dermatologist Cybele Fishman MD, says both green tea and pineapple contain antioxidants, elements that are under increased scientific scrutiny for treating acne.

According to physician assistant Angie Seelal, people going for a gel manicure, which requires exposure to UV light, should “swap the [hand] lotion for sunscreen” for protection before nail polish application.
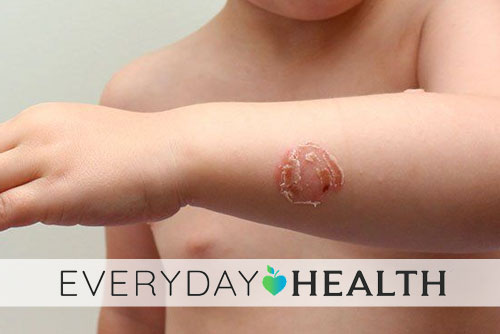
Impetigo isn’t usually anything to worry about when you treat it. Even scarring isn’t much of a concern unless your child scratches a lot, says Suzanne Friedler, MD.

Physician’s Assistant Angie Seelal, PA-C wants to clarify Head and Shoulders shampoo isn’t something to try if you’re simply dealing with a few blackheads.
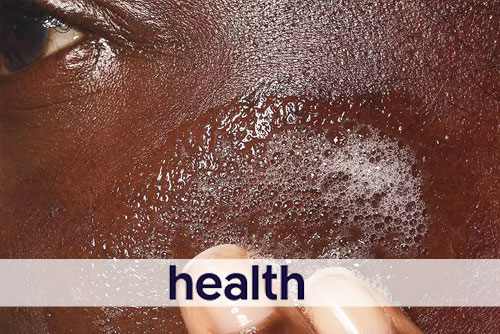
According to Cybele Fishman, MD people with skin conditions like rosacea and eczema should opt for non-foaming cleansers.

The U.S. Food and Drug Administration (FDA) considers tattoo ink to be a cosmetic. Angie Seelal, PA-C wants people to know that tattoos aren’t entirely risk-free.

Interview with Loretta Pratt, MD, about sneaky ways your hygiene routine works against you. And all you have to do is switch up a few small things, no purchases are required.

Dr. Loretta Pratt, a dermatologist at Advanced Dermatology PC commented on a study that tested the crib sheets for the best options for sensitive baby skin.

When it comes to small red bumps springing up on your body, there are many possible culprits. Suzanne Friedler, MD, a dermatologist with Advanced Dermatology PC gives us some dermatological possibilities.

People with diabetes are very prone to skin dryness, so Cybele Fishman, MD, a board-certified dermatologist recommends a few must-have products that will help bring some relief.

Say hello to thicker, shinier hair with these expert-approved products. Whether you’re pregnant or not (and even if you don’t intend to be!), your hair can benefit from a prenatal vitamins says Suzanne Friedler, MD

There’s no such thing as a safe or healthy tan, whether from the sun itself or from indoor tanning. Loretta Pratt, MD has several suggestions for products or techniques that can help us get that much-wanted glow.
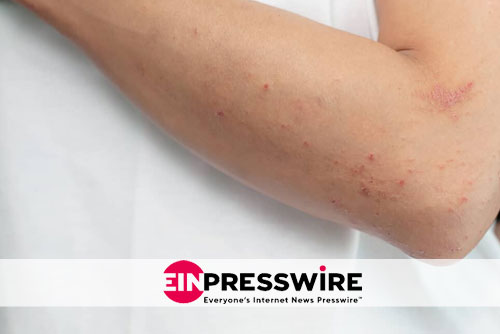
Some skin conditions are not as they appear. One of them is mycosis fungoides, a common cancer that “imitates” various skin conditions, says Jennifer Wong, PA-C with Advanced Dermatology PC.
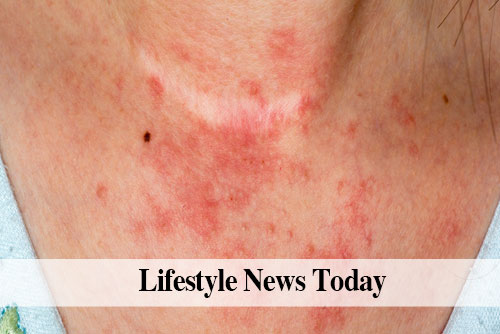
Almost all of us develop a red, itchy rash at some point, known medically as contact dermatitis, which can be triggered by a variety of causes and usually responds to several home measures, according to Christopher Byrne, PA-C.
Receive skincare tips, news and special offers!