Personalized Eczema Treatment at Advanced Dermatology P.C.
Also known as atopic dermatitis, eczema is a skin condition involving itching and inflammation. Although it can occur anywhere on the skin, eczema most commonly affects the arms and knees. Eczema is a chronic condition that flares up and subsides at random, making it difficult for those affected. At Advanced Dermatology, PC, we see many patients seeking treatment for this frustrating condition.
Eczema is a general term used to describe skin inflammation or “dermatitis.” Eczema is not contagious, but is believed to have a genetic component. It is therefore common for multiple members of the same family to have the condition. Research indicates that those with a family history of eczema or a family history of other allergic conditions, such as asthma or hay fever are more likely to present eczema. While eczema can affect people of any age, it is most common in infants. About 85% of people with eczema experienced its onset before the age of 5. Research shows that eczema is more common in females than males and effects people of all races.
There are several types of eczema and one can develop more than one type at the same time. Some of the most common types of eczema are Contact dermatitis, Dyshidrotic eczema, Nummular eczema, and Seborrheic dermatitis. (These different forms of eczema are discussed below under “What are some types forms Eczema?”)
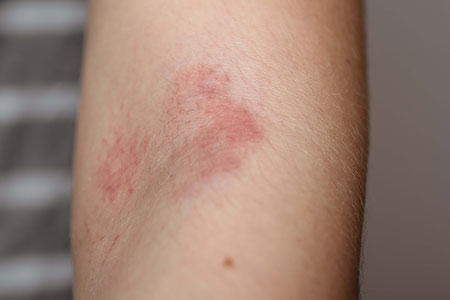
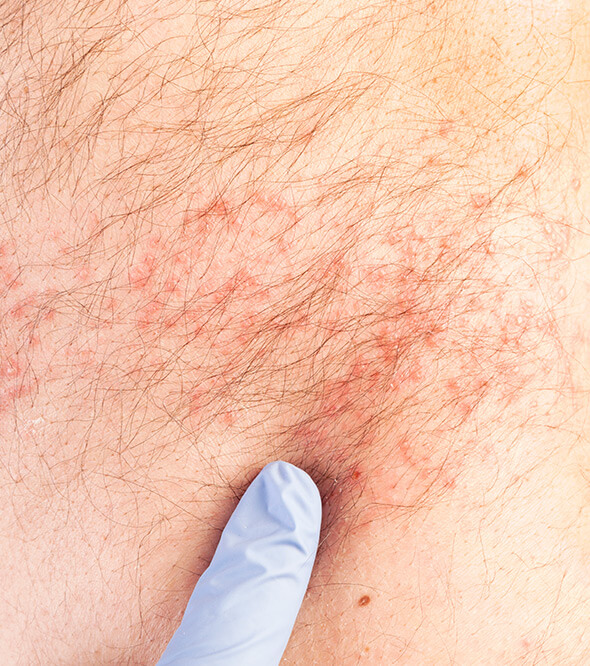
What Causes Eczema?
The actual “cause” of eczema remains a mystery, although it is likely a combination of irritable skin and a malfunction within the immune system.
Doctors and researches are continuously digging deeper into this condition to uncover the roots of the disease so that a cure can be developed. What is known about eczema is that some forms of the condition are triggered by substances that come in contact with the skin. Chemicals such as cosmetics, soaps and detergents, or even sweat and clothing, have been shown to trigger an eczema outbreak.
Environment may also play a role in eczema incidences, as studies show greater rates of eczema amongst children in cold regions, urban areas, or upper-class households. Eczema is hereditary, with studies show that individuals are at a heightened risk of eczema if one or more relatives have eczema, seasonal allergies, or asthma. Other events that have been shown to exacerbate eczema are high stress and anxiety.
Signs and Symptoms of Eczema
Different types of eczema (discussed below)present with different symptoms. Dry skin, reddened skin that itches or burns are the most common signs of eczema. Each individual case of eczema has the capacity to present in a unique manner, but in the most general terms, eczema usually brings on dry and scaly skin with an intense itching sensation that may be followed by blisters and oozing lesions. Repeated scratching of affected areas can lead to thickening and crusting of the skin. These symptoms can be brief and last for only a few hours or days, or can be chronic and persist for months and years. In both children and adults, eczema has the capability of presenting anywhere on the body. However, it is more common to find eczema on the face, neck, and the insides of the elbows, knees, and ankles. In infants, it is not uncommon to find eczema presenting on the forehead, cheeks, and forearms as well.
How to Diagnose Eczema?
Accurate diagnosis of any skin problem is the first step in treating the problem and preventing it from occurring again. Diagnosing eczema can be quite difficult, as this chronic skin condition can resemble a number of other skin problems. For this reason, it is important to consult with a dermatologist who experienced in diagnosing and treating eczema. With offices throughout NYC, Suffolk County, and Nassau County, our team of dermatologists has been helping patients manage eczema so that episodes of this painful disorder become less frequent and severe.
To diagnose eczema, our dermatologist will first talk to you about your medical history and the symptoms you have been experiencing. He will also examine your skin. Eczema is characterized by the presence of any of the following symptoms: itching and dryness, swelling, redness, discoloration, flaking, blistering or oozing, crusting, cracking, or bleeding. Itching skin is one of the most common problems associated with eczema. The need to itch may be so strong that the patients cannot control themselves or itch without conscious awareness. Scratching a lesion can result in scarring and further complications. If you are experiencing any of these symptoms on an ongoing or recurrent basis, eczema could be the culprit.
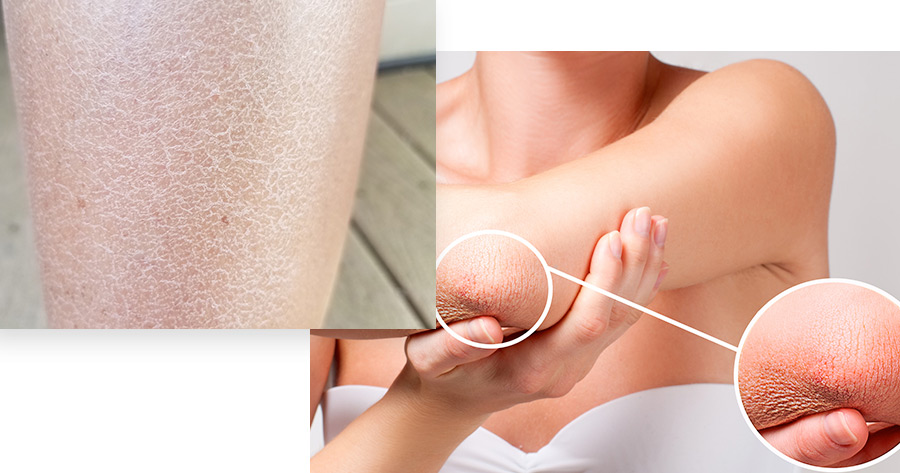
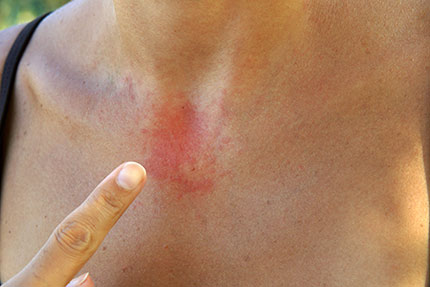
Eczema can appear differently in each person and its symptoms are easily confused with other disorders, such as contact dermatitis (a reaction to a substance that irritates the skin), psoriasis, or hives. As such, your medical history and the medical history of your family may help your doctor diagnosis eczema. The exact cause of this skin disorder is not known, but it is believed that eczema is caused by a combination of environmental and genetic factors. Eczema is considered to be part of a “trifecta” of chronic problems that includes asthma and seasonal allergies (hay fever). If you suffer from asthma and seasonal allergies, it is much more likely that your skin problem is eczema. Likewise, if family members suffer from asthma, rashes, and other allergy-related medical conditions, eczema is more likely to be diagnosed.
There are no specific tests that are used to diagnose eczema; however, our skin doctor may recommend that you undergo allergy testing in order to identify possible irritants or triggers. There is also no cure for eczema. Rather, the condition is one that is managed through a variety of medications, moisturizing routines, and/or lifestyle changes. Our dermatologists may observe how you respond to recommended treatments before giving a final diagnosis of eczema, as response or lack of response to certain medications may provide the doctor with a better idea of the condition.
Eczema is a complex and chronic skin condition that can make the sufferer’s life quite uncomfortable – but there is no need to continue suffering. By working with one of our experienced New York dermatologists, you can find relief from eczema and may be able to prevent future episodes from occurring. Don’t delay in seeking a diagnosis to any skin problem. This is a critical first step in regaining control and working towards healthier skin and a more comfortable life. With offices throughout NY, we are likely to have a location near you.
The first goal of an eczema treatment plan would be to prevent itching and reduce inflammation thereby minimizing the worsening of the condition. Treatment may involve changes in one’s lifestyle (to avoid allergens) and/or medication.
Avoiding products that may trigger an episode of eczema is the key to treating an existing condition and preventing a future episode. Keeping the skin well hydrated and moist is an important aspect in treating eczema. This can be accomplished by using oil based moisturizing creams. To treat inflammation, a dermatologist may prescribe a corticosteroid that helps reduce inflammation in the skin. Use of prescribed creams depends on the severity of the condition. A well-trained and qualified dermatologist will be advising you on the concentration of the cream and how often it should be applied. In severe cases, oral antihistamines may be prescribed. Phototherapy or light therapy is another form of treatment that is sometimes employed to treat people with eczema.
Types of Eczema
When dealing with a case of eczema, you may hear our doctors use an array of terms. As mentioned above, the word “eczema” is a broad term used to describe conditions of skin inflammation or “dermatitis.” Atopic Dermatitis is the most common form of eczema followed by Contact Dermatitis, Dyshidrotic Dermatitis, Hand Dermatitis, Neurodermatitis, Nummular Dermatitis, Occupational Dermatitis, Seborrheic Dermatitis, and Stasis Dermatitis.
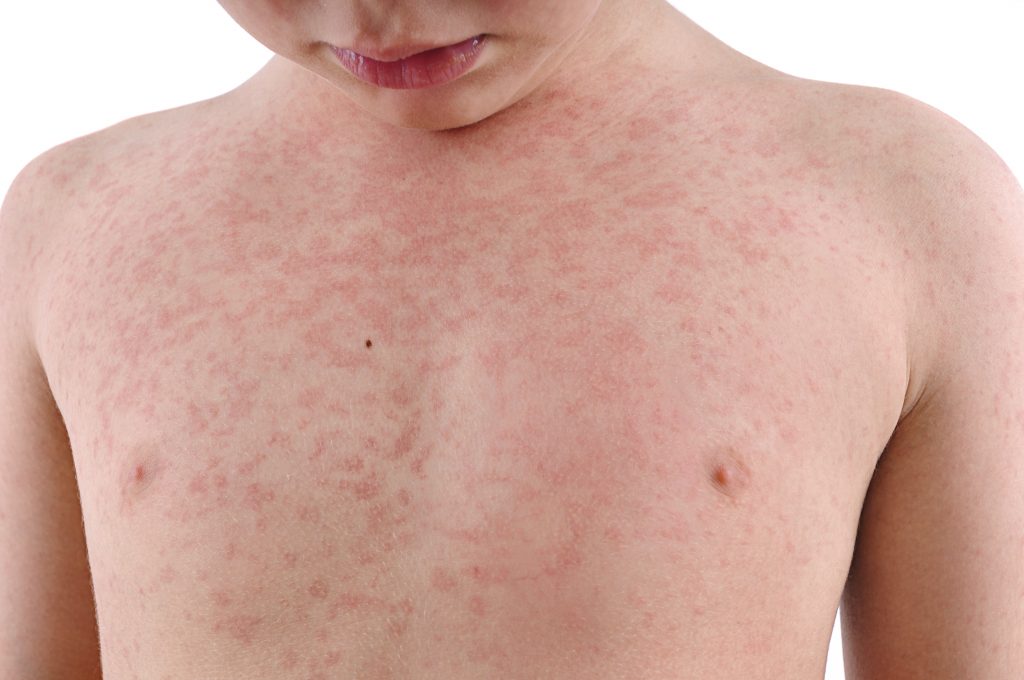
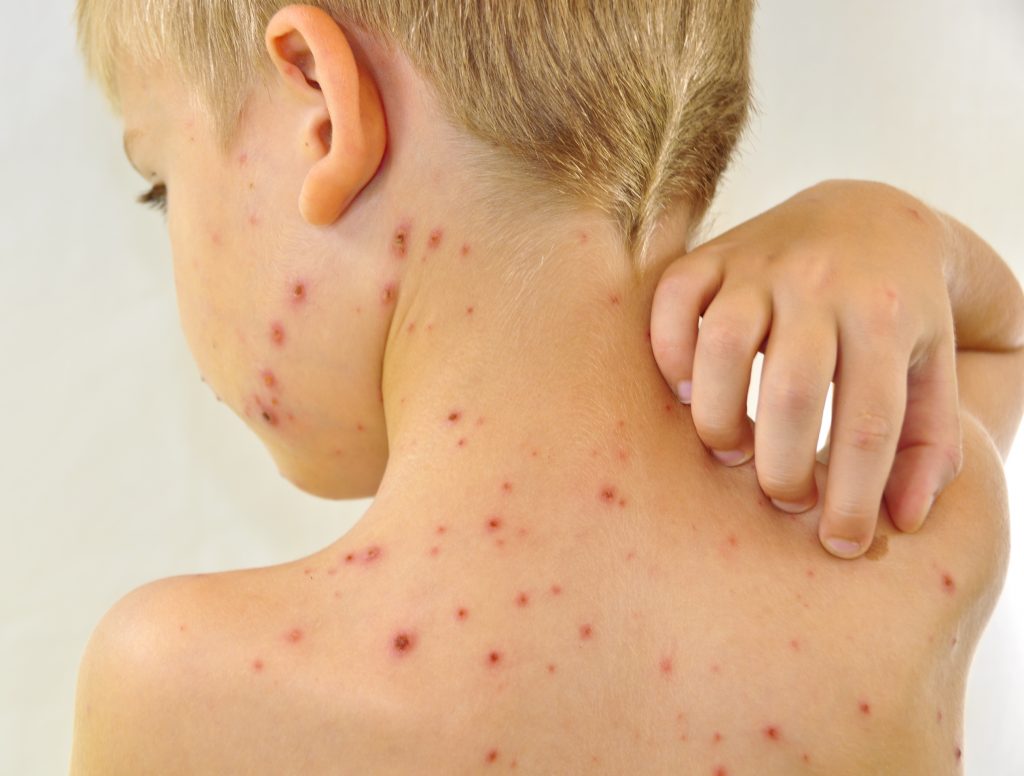
Atopic Dermatitis
Atopic dermatitis is a chronic skin disease that leads to eczema and is frequently described as “the itch that rashes.” It has been documented that a person’s quality of life can be affected due to the intense itching that atopic dermatitis brings on. When the disease presents in infancy, it is sometimes referred to as infantile eczema. Children are the most likely victims of this disease and often cannot sleep through the night due to the intense itch. This form of dermatitis has been shown to run down the family tree. A vast quantity of those presenting atopic dermatitis have a family history of the condition. Although it remains unclear as to what the cause of the condition is, dermatologists believe environmental factors such as mold, pollen, and pollutants play a role in triggering an episode of Atopic Dermatitis. Soaps, detergents, and perfumes are also believed to trigger the condition.
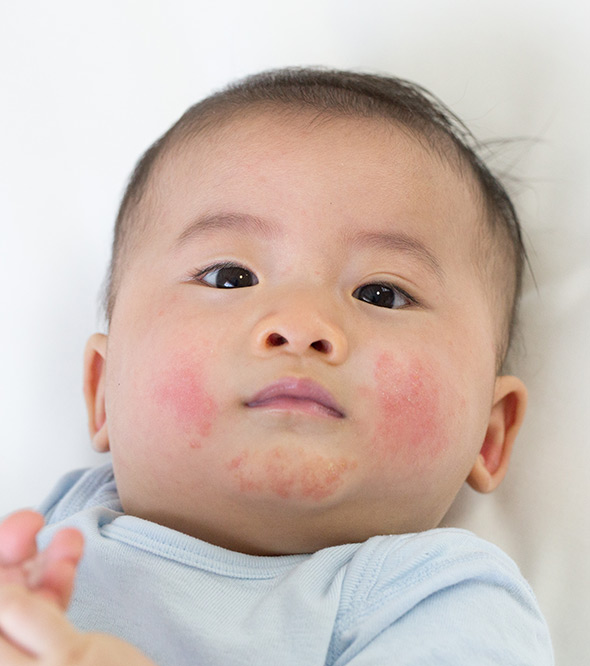

Contact Dermatitis
Contact Dermatitis or contact eczema is a localized reaction to an allergen. An allergen can be any object or substance a person came in contact with. From shampoo and jewelry to food and water, contact dermatitis brings along redness, itching, and burning in areas where the skin has come into contact with the allergen. Due to the vast number of substances with which individuals come in contact with on a daily basis, it can be difficult to determine the exact trigger for contact dermatitis. When the contact leads to irritated skin, the eczema is called irritant contact dermatitis. As with atopic dermatitismentioned above, it is very common to find that those with contact dermatitis have a family history of the condition.
Dyshidrotic Dermatitis
This form of eczema occurs on the palms of the hands, sides of the fingers, and soles of the feet. Dyshidrotic dermtitis typically causes a burning or itching sensation along with a blistering rash. In our office one may hear a doctor refer to this condition by a different synonym such as hand eczema, pompholyx, vesicular eczema, and vesicular palmoplantar eczema.
Hand Dermatitis
As mentioned above, there are several different and unique types of eczema. Hand eczema or hand dermatitis does not refer to one specific type of eczema, but rather is a broad and general name given to conditions of eczema that develop on the hands. The reason hand eczema is given specific attention by medical professionals is because hand eczema is often the result of one’s occupation. The allergy a person has may be directly related to their specific occupation.
Neurodermatitis
Neurodermatitis, as its name implies, stems from a condition in the body’s nervous system. This form of dermatitis arises when nerve endings in the skin become irritated, triggering a severe itch-scratch-itch cycle. Patients with this condition report that endless scratching does little to relieve the itching sensation of the condition. Common causes of nerve irritation include an insect bite and emotional stress. Women are more likely to develop Neurodermatitis than men. The condition generally will present itself between the ages of 25 and 50 and can result in thickened and leathery skin.
Nummular Dermatitis
Nummular Dermatitis is a common form of dermatitis that develops after the skin experiences trauma (skin injury such as a burn, abrasion, or insect bite). That being the case, the most common areas that develop nummular dermatitis are arms, knees, legs, and buttocks. The hallmark of this condition are unique coin-shaped (nummular) or oval lesions and patches of irritated and itchy skin.


Occupational Dermatitis
Occupational dermatitis is not limited to one specific form of eczema. Rather, it is any type of eczema caused by a person’s workplace or occupation. This distinct classification came about because occupational dermatitis has unique causes and many people develop eczema on the job.
Seborrheic Dermatitis
Seborrheic dermatitis generally presents on the scalp as oily and waxy patches. It is not uncommon for this form of dermatitis to spread to the face, cheeks, and shoulders. Seborrheic dermatitis does not necessarily have the “itching sensation” that come along with other forms of eczema. As mentioned previously, seborrheic dermatitis has a tendency to flare up when exposed to triggers such as cold temperatures and dry weather. Our doctors may use synonyms such as Cradle Cap (occurs in infants aged 0 to 6 months), Dandruff, and Seborrhea when referring to this condition.
Stasis Dermatitis
Stasis dermatitis occurs almost exclusively in middle aged people. As one ages, circulation in the lower extremities such as the legs begins to slow. Diminished blood flow to the lower extremities can lead to a fluid build up. This ultimately leads to swelling that affects the skin by causing an itchy rash with painful sores and skin discoloration. To effectively treat this form of dermatitis, our doctors will not only take into account the trauma to the skin, but will focus on correcting the circulation problem thereby diminishing the swelling which will ultimately terminate the skin condition.
Can Eczema Be Prevented?
As mentioned above, it is not completely clear as to what the cause of eczema is but there are certain measures that can be taken to prevent an outbreak or a reoccurring episode. Exercising good skin hygiene is a first step in both preventing and treating eczema. Keeping the skin moist is an excellent preventative measure. Bathing or showering with a mild soap and shampoo that does not dry the skin out, and applying a moisturizer after bathing and showering will help prevent an episode of dermatitis. Those that have experienced an episode of dermatitis should limit or avoid contact with known irritants like soaps, perfumes, detergents, and jewelry. Instead of itching and irritating the skin, one should use a cold compress to control the uncomfortable sensation and should visit a dermatologist to determine a treatment plan.
Tips to Control Eczema
Eczema is a chronic skin condition that can cause severe itching, pain, and swelling. Fortunately, there are a number of ways that you can gain control over this disorder and experience a more comfortable life. Eczema can be controlled by managing symptoms when they occur and by finding ways to prevent or decrease the occurrence of eczema episodes. Each person experiences eczema differently; therefore, a solution that provides relief for one person, may not be helpful for another. As such, it is important that eczema sufferers find an experienced dermatologist to support them as they manage their condition. Our team of dermatologists has been helping eczema patients throughout NY and NJ improves the quality of their lives through proper eczema management.
From our many years of treating people in New York City, New Jersey, Suffolk County, and Nassau County, we have developed a number of strategies for controlling eczema. Drawing on that knowledge, we have put together the following set of tips and recommendations to help control eczema.
Know and avoid your triggers
Try to figure out what triggers or worsens an episode of eczema (your doctor can help). Once you understand what causes a flare up, you will be more in control of your condition. Common ingredients in many household products, such as soaps, toothpaste, fabric softeners, may worsen your eczema. Many eczema sufferers also suffer from seasonal and food allergies, which may exacerbate your condition. You may wish to undergo allergy testing so you can become aware of such triggers and avoid them.
Avoid allowing your skin dry out
The ingredients in most conventional soaps and shampoos can cause the skin to dry out. Try using a hypoallergenic wash or forgoing soap altogether. Hot baths and showers will also dry out the skin, so it’s best to bathe in lukewarm water. Your doctor may recommend that you bathe more or less frequently, depending on your unique case.
Keep your skin moisturized
Regularly apply an emollient-rich moisturizer to you skin at least three times a day. Avoid using lotions, creams, or ointments that contain fragrances and other common irritants. In general, look for a product that contains only a few ingredients, as this will help you identify and avoid known triggers more easily. Some people use oils (such as olive or avocado oil) to control their eczema. You may find this helpful, but be sure that you are not allergic to any of the ingredients first. In order for the moisturizer to be effective, your skin should be damp. Apply moisturizers directly after bathing, or dampen your skin before applying the moisturizer.


Minimize itching
In order to allow your skin to heal, you must avoid the itch-scratch cycle. Routine moisturizing can help prevent itchiness, but there will be times when you feel itchy even after preventative measures. In these cases, speak with your doctor about the types of medications you can use to safely control itching sensations and prevent scratching your skin. These medications may include an over-the-counter hydrocortisone cream or anti-inflammatory tablets. For more severe cases, your doctor may prescribe something stronger.
Regulate your living environment
Extreme temperature and humidity changes in your home may cause an eczema flare up. Use air conditioning, heating, and a humidifier to regular the conditions inside of your home, as recommended by your doctor.
Ointments may be better than creams
Many dermatologists recommend that their patients use ointments rather than creams. Ointments consist of 80% oil or more, while creams and lotions contain less than 50%. Thus, ointments tend to be better moisturizers and are more effective at sealing in moisture and creating a protective barrier around your skin. The key, however, is to actually use the moisturizers, so if a heavy ointment prevents you from going about your normal routine and deters you from applying any moisturizer, then it’s not the right choice for you.
Use antibiotic ointment on cracked skin
If your skin routinely cracks from eczema, you may wish to apply an over-the-counter antibiotic ointment to prevent infection of the affected skin.
Keep your nails trimmed and hands clean
Because scratching may be unavoidable or uncontrollable (for example, during the night), you can help yourself by keeping your nails short to avoid severely scratching your skin. Keep your hands clean to prevent infection in the event that you scratch to the point of bleeding. You may also wish to consider wearing soft gloves to bed at night to prevent nighttime scratching.

What Causes Eczema Flare-Ups?
Those living with eczema will at some point in time try to get to the bottom of what causes eczema flare-ups. Every person has different triggers, so there is no easy answer. But common triggers include:
- Dry skin
- Certain fabrics (like wool or polyester)
- Pet fur or dander
- Harsh soaps
- Stress
- Temperature changes
- Anything on the list of common allergens like cigarette smoke or perfumes
Flare-ups can be treated with over-the-counter or prescription creams to reduce itching and prevent further outbreaks. Ultraviolet therapy done in a dermatology office may also be of benefit. Oral antihistamines, steroids, or other systemic medications may be needed. It may take some time to figure out the treatment or combination of treatments that works best for you.
Eczema treatments:
- Topical creams, such as corticosteroids (severe) and hydrocortisones (mild), to reduce inflammation
- Immunomodulator creams that control inflammation and immune system reactions
- Systemic pills that suppress the immune system
- Prescription strength moisturizers that restore the skin barrier
- Oral antihistamines to relieve inflammation
- Diluted bleach baths and antibiotics to treat infection

Frequently Asked Questions
What is the main cause of eczema?
There are many different factors that cause eczema, but in most cases, it seems to be related to an overactive immune system. When exposed to certain substances or foreign elements, this overactive response by our defenses is what produces inflammation of the skin and other symptoms of this condition.
What does eczema look like?
The appearance of eczema can vary greatly depending on the severity of the condition. In mild cases, the skin looks dry, has a rough texture, and you may see visible flaking on the surface. In severe forms, eczema can cause the skin to crack, ooze, and have an intense red color.
How can you clear up eczema?
While eczema can be caused by a variety of factors, there is a handful of home remedies you can try before seeking medical assistance. If you have mild eczema, you may address it by taking a warm bath or shower and moisturizing with a chemical-free product immediately after you step out of the bathroom.
What foods trigger eczema flare-ups?
Some foods have been related to the development of eczema. These are usually allergens like fish, wheat, milk, soy, peanuts, and eggs. In order to test different foods and identify mild allergies that are causing eczema outbreaks, your best bet is to consult with a board-certified dermatologist and skincare expert in your area.
What are the first signs of eczema?
The very first signs of eczema are intense itching and dryness. In some cases, you will see a rash. Red bumps of different sizes may also start appearing. If you scratch your skin, it may become oozy and flaky, intensifying the pain.
