Actinic Keratosis Treatment in NY, NJ & CT
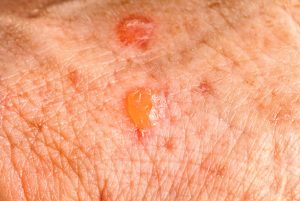
Actinic keratosis (AK), also known as solar keratosis, by far the most common precancer, is the result of prolonged exposure to sunlight. It is a small crusty or scaly bump or horn that arises on or beneath the skin surface. The base may be light or dark, tan, pink, red, or a combination of these … or the same color as your skin. The scale or crust is horny, dry and rough, and is often recognized by touch rather than sight. Occasionally it itches or produces a pricking or tender sensation. It can also become inflamed and surrounded by redness. In rare instances, actinic keratoses can bleed.
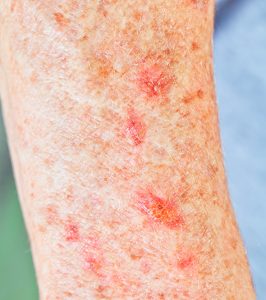
The skin abnormality or lesion develops slowly and usually reaches a size from an eighth to a quarter of an inch (2mm to 4mm) but can sometimes be as large as one inch. Early on, it may disappear only to reappear later. It is not unusual to see several AKs at a time. AKs are most likely to appear on the face, lips, ears, scalp, neck, backs of the hands and forearms, shoulders and back – the parts of the body most often exposed to sunshine. The growths may be flat and pink or raised and rough.
Actinic keratoses can be the first step leading to squamous cell carcinoma (SCC). Some studies show that ten percent do advance, and 40-60 percent of SCCs begin as untreated AKs.
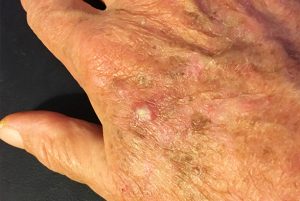
Treated early, almost all actinic keratoses (AKs) can be eliminated before becoming skin cancer. There are many effective methods for removing AKs, and the choice is determined by many factors, including the location, type and size of the lesion, and also the health, age and preference of the patient and the preference and experience of the physician. For example, a treatment that has a high cure rate and is painless but leaves a large scar might not be preferred for a tumor on the face.
Almost all treatments can be performed in the physician’s office. Before selecting a treatment, the physician takes a biopsy specimen to test for malignancy. This is done by shaving off the top of the lesion with a scalpel or scraping it off with a curette. Then the curette is used to remove the base of the lesion. Bleeding is usually stopped with a styptic agent. Local anesthesia is required.
Cryosurgery
The most common treatment for AKs, it is especially effective when a limited number of lesions exist. Liquid nitrogen is applied to the growths with a spray device or cotton-tipped applicator to freeze them. They subsequently shrink or become crusted and fall off, without requiring any cutting or anesthesia. Some temporary redness and swelling may occur after treatment, and some pigment may be lost.
Chemical Peeling
This method makes use of trichloroacetic acid (TCA) or a similar agent applied directly to the skin. The top skin layers slough off and are usually replaced within seven days by new epidermis (the skin’s outermost layer). This technique requires local anesthesia and can cause temporary discoloration and irritation.
Laser Surgery
A carbon dioxide or erbium YAG laser is focused onto the lesion, removing epidermis and different amounts of deeper skin. This finely controlled treatment is an option for lesions in small or narrow areas; it can be effective for keratoses on the face and scalp, as well as actinic cheilitis on the lips. Laser surgery is useful for people taking blood thinners and is also a secondary therapy when other techniques are unsuccessful. However, local anesthesia is usually necessary, and some scarring and pigment loss can occur.
Topical Medications
Medicated creams and solutions are especially useful in removing multiple lesions and those beneath the surface of the skin. The patient applies the medication according to a schedule worked out by the physician. The doctor will also regularly check progress. After treatment, some discomfort may result, but the risk of scarring is minimal.
5-fluorouracil (5-FU) cream or solution, in concentrations from 0.5 to 5 percent, is the most widely used topical treatment for AK. It works well on the face, ears and neck and has FDA approval. Redness and irritation occur, but final cosmetic results are good.
Imiquimod cream, also FDA approved, works by stimulating the immune system. It causes cells to produce interferon, a naturally-occurring chemical that destroys cancerous and precancerous cells. Redness and irritation are side-effects for this agent, too, and final cosmetic results are good.
An alternative treatment, a gel combining, hyaluronic acid and the anti-inflammatory drug diclofenac, also may prove effective.
For more information, please visit our offices located in Manhattan, Bergen County, Long Island, Queens and more.
Photodynamic Therapy (PDT)
PDT can be used to treat lesions on the face and scalp. Topical 5-aminolevulinic acid (5-ALA) is applied to the lesions by the physician. The next day, the medicated areas are exposed to strong light that activates the 5-ALA. The treatment selectively destroys actinic keratoses, causing little damage to surrounding normal skin, although some swelling and redness often occur.
Frequently Asked Questions
What is the best treatment for actinic keratosis?
All patients are unique, so the best treatment for actinic keratosis will vary based on different factors. These include the location of the skin condition and its size as well as the current health, and age of the patient. In order to achieve the best results, you should consult with dermatology and skin care professionals as soon as you notice any potential symptoms.
Is actinic keratosis cancerous?
Although actinic keratosis is not cancerous, it can turn into squamous cell carcinoma or SCC if left untreated. To prevent this from happening, make sure you consult with a certified dermatologist and consider all the different elements that may be causing the skin lesion.
What causes actinic keratosis?
There are many different factors that influence the development of actinic keratosis. These lesions usually appear in areas that have been exposed to sunlight for decades, like the face, back of the hands, and back of the neck. However, other elements can also impact the onset of these lesions, like skin health and age, to name a few.
Is actinic keratosis dangerous?
Actinic keratoses can cause itchiness, discomfort, and make your skin look unhealthy. Additionally, if left untreated, actinic keratosis can develop into a type of cancer called squamous cell carcinoma.
Is actinic keratosis always scaly?
In most cases, actinic keratosis appears as scaly, patchy bumps that have a rough texture. However, in other instances, it may not be visible to the eye despite being able to feel the coarse texture. Furthermore, if left untreated, the lesion slowly grows so you have to work with a seasoned dermatologist to eliminate it completely.
