Do your feet hurt? Let’s start with where. Your foot may seem like a small part of your body, but with 28 bones, 36 joints, plus over a hundred different muscles, tendons, and ligaments, there’s a lot of places for something to go wrong. It is no wonder that 19% of men and 25% of women experience foot pain limiting their function. Foot pain can be pretty debilitating, leading to problems working and affecting happiness and overall well-being. Here we talk about some common causes of foot pain and what we can do about them.
Bunion
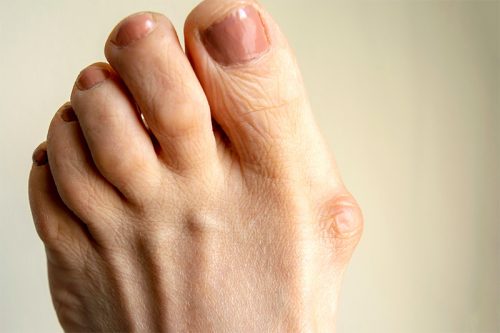
What’s a bunion? A bunion is a structural deformity with the first metatarsal that causes a bump on the side of the foot behind your first toe. This bump forms when the first toe turns towards the second toe and the metatarsal turns in the opposite direction. This bunion is often painful and can lead to difficulty wearing shoes, sub-optimal function when walking and running, and degenerative arthritis. Signs of a bunion are the characteristic bump with redness, soreness, and stiffness in the big toe joint.
Many things can contribute to or cause a bunion to form, including tight shoes, genetics, overuse, congenital deformity, and inflammatory arthritis such as rheumatoid arthritis. We use X-rays to help determine the severity of the bunion deformity and the best treatment options. Thankfully, there are various ways to treat bunions and the pain associated with them—these range from conservative options that involve changing shoe gear, orthotics, and injections to surgical correction. Depending on the severity and x-ray findings, various surgical procedures can be performed, including bone shaving, bone cutting, realignment, or even joint fusions.
Hammertoe
What’s a hammertoe? A contracture (or bending) of the lesser toe joints into a fixed position is known as a hammertoe. These can become unsightly and painful, contributing to corn or callus formation. An imbalance in the foot’s musculature can cause hammertoes, where the tendons on the bottom of the toes overpower those on the top. Sometimes the toe becomes permanently bent in this flexed position, and wearing shoes becomes painful when the top of the toe is rubbing against the inside of a closed-toe shoe. With constant rubbing in the area causing friction, calluses and corns will develop. A lot of times, it is faulty biomechanics in your feet that cause hammertoes. Some people are genetically predisposed to developing hammertoes, some are caused by activity and ill-fitting shoe gear, and some people are just born with them.
As with bunions, X-rays are a mainstay in properly evaluating hammertoes and determining the best treatment options. Treatment starts with determining the actual biomechanical cause of the contracted toe. It ranges from conservative care to alleviate the pain, such as anti-inflammatory medications, shoe gear changes, orthotics, shaving down corns and calluses, to surgical correction. Surgery is typically very well tolerated and has various options depending on the type and severity of hammertoe. These include tendon transfers, toe fusions, or shortening the toe to hold it in a corrected position. The recovery period for a hammertoe correction usually involves four weeks in a boot.
Metatarsalgia
Metatarsaglia is a pain in the “ball” of your foot where the metatarsal bones are. Pain and inflammation in this area can have several causes. Overuse from physical activity, certain foot types, and poor shoe gear or fit are common culprits. When increased pressure from tight-fitting shoes or a high arched foot occurs in the metatarsal joints with your toes, inflammation occurs, known as capsulitis. Capsulitis can also occur in feet that are biomechanically unstable or where the first metatarsal is shorter than it should be, and the weight of the body is not distributed evenly across all metatarsals. Bunions, hammertoes, obesity, and age-related fat pad atrophy are all common causes of metatarsalgia.
When treating metatarsalgia, determining its cause is critical, and x-rays or advanced imaging can help with this. Changing shoe gear to those that properly fit and have a wider toe box can help, and so can modifying your activities. Orthotics to improve biomechanical function and offload the high-pressure area are also very effective. Cortisone injections and anti-inflammatory medications relieve pain and inflammation. If the condition is secondary to a deformity such as a bunion, hammertoe, or short 1st metatarsal, surgery to correct these are necessary and will result in pain relief.
Heel and Arch Pain
Do your heels or arches hurt? Pain in the arches and heels is one of the most common problems a podiatrist will see. Pain on the bottom of the heel or along the arch on the “inside” of the foot could be due to Plantar Fasciitis. The plantar fascia is a large ligament that runs from your heel bone down the bottom of the foot to the base of your toes and supports your foot. If this ligament is tight, it can pull on its insertion on the heel when you step down, causing inflammation and pain. If the pain is very severe, the plantar fascia may be torn. Over time, a heel spur can form due to the tightness and pulling on the heel bone.
Typically, people will say they have pain when they step out of bed in the morning, sit down, or stand on their feet all day. Having a tight Achilles tendon will worsen this problem, as the Achilles tendon also inserts on the heel bone. Treatment involves adding a heel lift to shoes, orthotics, anti-inflammatory medications, and corticosteroid injections. These combined with daily active stretching exercises or physical therapy often do the trick. Plantar fascia tears are treated using a walking boot for four weeks, followed by physical therapy. Persistent plantar fasciitis, which is rare, can be treated with several surgical approaches.
Mass or Lump
Is there a painful mass or lump on your foot? These can be tricky when wearing closed shoes that rub against them. Where is it? If it’s on the top of the foot, it could be a ganglion cyst. Ganglion cysts are fluid-filled sacs that form off of the lining of a joint or tendon. Trauma or chronic irritation causes these, inflicting inflammation, pain, and sometimes numbness. These can be aspirated in the office, and a corticosteroid injection can prevent them from recurring. Other times your podiatrist can remove them surgically.
If the mass is on the bottom of your foot along your arch, it could be a plantar fibroma. A fibroma is a benign tumor within the plantar fascia ligament, caused by injury or inheritance, causing pain and discomfort when walking or wearing particular shoes. To help alleviate the pain, anti-inflammatory medications and corticosteroid injections, as well as orthotics, are helpful. Certain topical medications containing a calcium channel blocker have also been shown to be beneficial. Surgical excision of plantar fibromas that fail conservative treatment is also an option.
Another cause for a mass or lump on the foot could be a boney exostosis. A boney exostosis is an outgrowth that usually occurs near a joint. These can cause the area to become painful, inflamed, and even discolored if shoe gear is causing constant friction. In some instances, an arthritic joint might be the culprit. Anti-inflammatory medications, corticosteroid injections, orthotics, and surgical removal are all options for treating these.
Fractures
Did you overdo it training over the weekend? Stress fractures, also known as hairline fractures, are particularly painful and notoriously difficult to see in X-rays. These injuries are usually from overuse and fatigue and are very common in the second metatarsal in runners. Swelling and pain located to a specific area over the bone can be a sign of stress fracture. Stress fractures can usually be treated using a walking boot for six weeks.
Toe fractures and other fracture types have varying degrees of severity, and this determines treatment. Signs of a fracture would be persistent pain and swelling with difficulty or inability to bear weight following an injury. If you are experiencing this, X-rays are highly recommended to evaluate the injury. Fractures can sometimes be reduced and splinted and sometimes require surgical open reduction with internal fixation. Luckily, the bone usually takes only 6-8 weeks to heal.
Whether experiencing acute pain from overdoing it on a run or pain from walking or standing during the day, it is a good idea to be evaluated by a podiatrist. This way, they can identify exactly what is causing the pain and get your feet back up and running. Make your appointment today!