Melasma: Symptoms, Causes and Treatment Options
If you’ve noticed dark, even patches on your cheeks, forehead or upper lip, you may have melasma, a common skin disorder. It can be frustrating, but it is very treatable.
At Advanced Dermatology, P.C., our board-certified dermatologists have helped thousands of patients across New York and New Jersey manage this condition with personalized, evidence-based skin discoloration treatment.

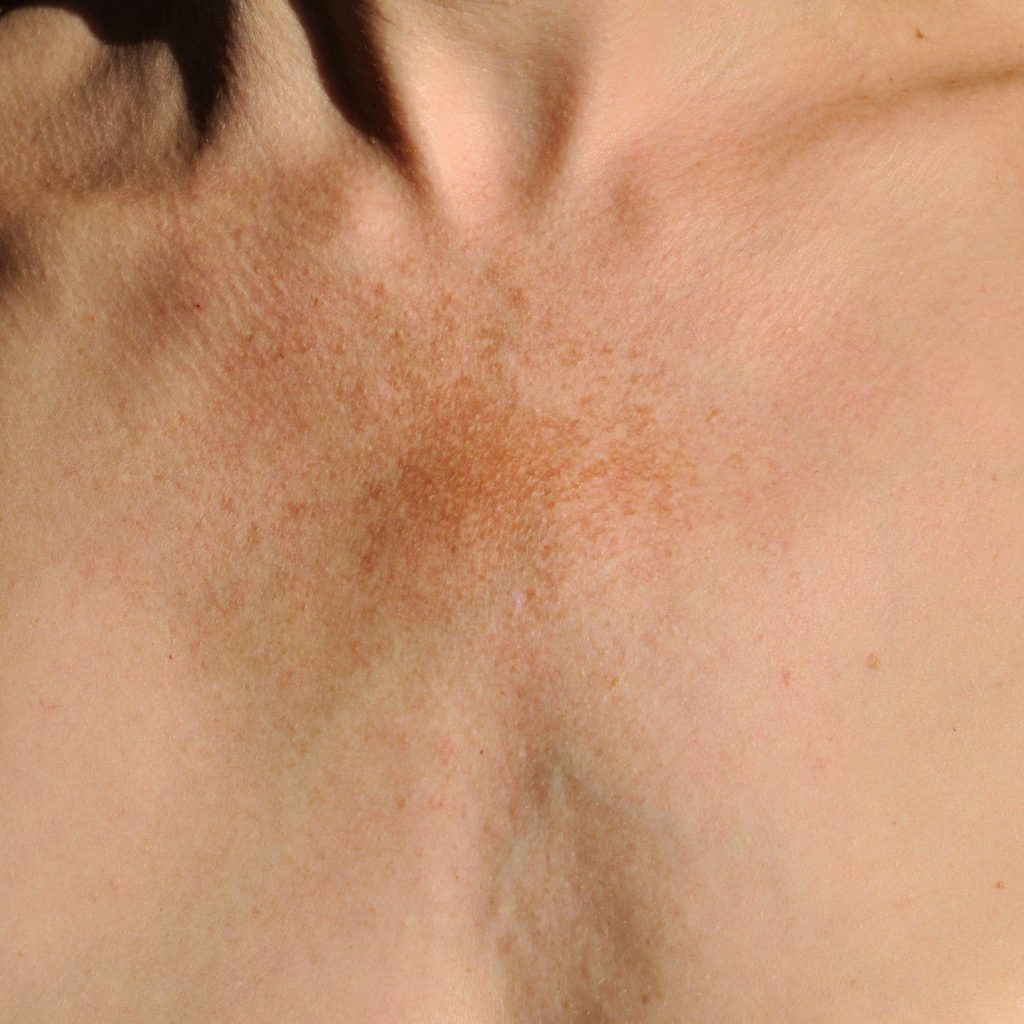
What Is Melasma?
Melasma is a pigmentation disorder, not a rash, not a sign of cancer and not contagious.
Melasma happens when the cells that give skin its color (called melanocytes) make too much pigment and spread it unevenly. This leads to dark, patchy areas that many patients find upsetting. The American Academy of Dermatology recognizes it as one of the most commonly treated pigmentation conditions in dermatology.
It most often shows up on sun-exposed areas of the face and tends to come and go over time. Several things can trigger it, including sunlight, hormones and genetics. Managing melasma means controlling it over time, not just clearing it once.
Where Does Melasma Appear?
Melasma most commonly appears on the cheeks, nose, chin, upper lip and forehead. It can also affect the arms, neck and back, especially skin that gets a lot of sun. This is why symptoms often get worse in summer.
What Does Melasma Look Like?
Melasma shows up as wide, flat patches (brown, gray-brown or bluish gray) with soft, blurred edges. A defining feature is symmetry: if it appears on one cheek, it almost always appears on the other. It is grouped into three types (epidermal, dermal and mixed) based on how deep the pigment is, which helps guide treatment planning.

What Causes Melasma?
The exact cause of melasma is not fully understood, but research consistently points to sun and visible light exposure, hormonal fluctuations and genetic predisposition. New research shows that melasma involves several types of skin cells, not just melanocytes, which helps explain why it often comes back.
Sun Exposure and UV Radiation
Sun exposure is one of the biggest triggers. UV rays signal your body to make more melanin, which is why melasma often shows up on the face, neck and arms.
Research published in the Journal of Clinical Medicine shows that visible light, including the blue light from screens, can make melasma worse. This means protection involves more than just wearing sunscreen outdoors.
Hormonal Triggers
Hormonal changes are a major driver of melasma. Rising estrogen and progesterone during pregnancy are thought to trigger it, which is why melasma is sometimes called the “mask of pregnancy.” Birth control pills and hormone replacement therapy can have a similar effect.
Genetic Predisposition
If a close family member has melasma, your chances of developing it are higher. It is also more common in people with medium to dark skin tones and in women of Latin, Asian, Black or Native American heritage. The American Academy of Dermatology confirms that family history is one of the strongest risk factors.
How Is Melasma Diagnosed?
In most cases, a dermatologist can diagnose melasma by looking at the skin. A visual exam is usually enough, though other tools may be used to rule out similar conditions.
A Wood’s lamp is a special UV light that helps reveal how deep the pigment sits in the skin. This matters because shallow melasma responds differently to treatment than deeper melasma. A skin biopsy is rarely needed but may be used if there is any doubt about the diagnosis.
A dermoscope, a handheld magnifying tool, can also help tell melasma apart from other pigmentation disorders.
How Is Melasma Different from Other Pigmentation Conditions?
Melasma can look similar to other skin conditions, but they are not the same. Treating the wrong condition can make things worse. Here is how melasma differs from the most common look-alikes.
- Melasma vs. Sunspots
Sunspots are caused by years of UV exposure and are not linked to hormones. They tend to have sharper, more defined edges and stay consistent year-round. Melasma, by contrast, has softer edges, appears symmetrically on the face and tends to flare with hormonal changes and heat. - Melasma vs. PIH
Post-inflammatory hyperpigmentation (PIH) is the dark mark left behind after a skin injury or breakout, such as acne or eczema. It can appear anywhere on the body. Melasma is driven by hormones and largely forms on the face. - Melasma vs. Vitiligo
Vitiligo causes patches of skin to lose color and turn white, which is the opposite of melasma. While melasma results from overactive pigment cells, vitiligo results from those cells being destroyed.
There are several other conditions that can look like melasma, which is why a proper diagnosis from a board-certified dermatologist is so important before starting any treatment.

Treatment Options for Melasma
There is no single fix for melasma, but there are many effective cosmetic dermatology options. We create each treatment plan based on your skin tone, how deep the pigment is and what may be triggering it. A 2024 analysis shows that sun protection, topical treatments and in-office procedures are still the most common and well-studied ways to treat melasma.
Topical Treatments (Hydroquinone, Retinoids, Vitamin C)
Prescription creams are usually the first step. Hydroquinone is the most commonly prescribed option and works by slowing down melanin production. It is often combined with tretinoin (a retinoid) and a mild steroid in an FDA-approved “triple combination” cream.
Vitamin C is another effective ingredient that helps block pigment formation and protect against UV damage. For patients who cannot tolerate these, alternatives like azelaic acid, kojic acid and niacinamide are available.
Chemical Peels
Chemical peels work by removing the top layers of skin to reduce pigmentation and encourage fresh skin to grow in its place. Glycolic, salicylic, trichloroacetic (TCA) and lactic acid peels are all options for melasma. Our providers choose the right peel strength for your skin to improve results while lowering the risk irritation or darkening.
Laser Therapy (Fraxel, MedLite®)
When creams and peels are not enough, laser therapy is an option. Fraxel laser treatment is the only laser with FDA approval specifically for melasma and works well for surface-level pigmentation.
The MedLite laser is another option, particularly for deeper or more stubborn cases. We often recommend using hydroquinone cream for a few weeks before laser treatment to lower the risk of side effects.
IPL (Intense Pulsed Light)
IPL uses broad-spectrum light to target pigment in the skin while leaving nearby tissue unaffected. Because it covers a wide range of wavelengths, it can treat both surface and deeper pigmentation at the same time. It works well on its own or in combination with other therapies.
Sun Protection as Ongoing Management
No treatment plan for melasma works without daily sun protection. Sun exposure increases melanin, which can darken existing patches and trigger new ones. We recommend wearing a wide-brimmed hat, staying in the shade when possible and applying a broad-spectrum SPF 30+ sunscreen every single day, even when it is cloudy.
Frequently Asked Questions
Can melasma go away on its own?
Sometimes. If a hormonal trigger like pregnancy or a birth control pill is the cause, melasma may fade once that trigger is removed. But it can also stick around for years, especially if sun exposure continues. Melasma is harmless, but many people choose to treat it for cosmetic reasons. We recommend getting evaluated sooner rather than later, as long-standing melasma can be harder to clear.
Is melasma the same as hyperpigmentation?
No, melasma is a form of hyperpigmentation. Hyperpigmentation is a general term for any darkening of the skin. What sets melasma apart is its hormonal component, its symmetrical appearance on the face and how easily it comes back.
Does melasma come back after treatment?
Yes, it can. Melasma is a chronic condition. Treatments can fade it significantly but rarely eliminate it for good. Recurrence is one of the most common challenges in melasma care. That is why we always build a long-term maintenance plan into every patient’s treatment, not just a short-term fix.
What is the best sunscreen for melasma-prone skin?
For melasma patients, a tinted sunscreen is the best choice. Regular sunscreens block UV rays but do little to protect against visible light, which is also a trigger for melasma flares. A 2025 review in Photodermatology, Photoimmunology & Photomedicine found that tinted sunscreens with iron oxides block both UV and visible light at rates above 93% and can even boost the effectiveness of hydroquinone. We recommend a tinted, broad-spectrum SPF 30+ sunscreen with iron oxides, worn every day.
Can men get melasma?
Yes. While melasma is far more common in women, a 2018 study published in the Journal of Clinical and Aesthetic Dermatology found that about 10% of cases occur in men, and were more common in men of Asian, Indian and Hispanic origin. In men, it tends to be linked more to sun exposure and family history than hormonal changes.
Schedule a Melasma Consultation at Advanced Dermatology, P.C.
With more than 40 locations across New York and New Jersey, expert care is easy to access. Whether this is your first time dealing with melasma or you have been struggling with it for years, we are here to help.
Find the Advanced Dermatology, P.C. location nearest you and book an appointment today.
