Fungal skin infection treatment
At Advanced Dermatology, P.C., we offer high-quality care for a wide range of fungal skin infections.
Our experienced team is dedicated to diagnosing and treating conditions such as ringworm, tinea versicolor, and toenail fungus, ensuring every patient receives expert care and effective solutions for healthy, comfortable skin and nails.
Fungal infections overview
Fungal skin infections are common problems that affect people of all ages. According to data published in 2025 by the National Library of Medicine, there were 1.73 billion cases of skin fungal infections globally.
Fungal skin infections can cause discomfort, itchiness, and changes in the appearance of your skin or nails. Understanding the types, causes, and treatments for fungal skin infections can help you protect your skin and stay healthy.
At Advanced Dermatology, P.C., we offer comprehensive dermatological care for a variety of skin conditions, helping patients achieve exceptional, long-term results.
What are fungal infections?
Fungal infections are caused by microscopic organisms called fungi. These fungi live in the environment, including on your skin, and can sometimes grow out of control, leading to infection.
Common examples include ringworm, tinea versicolor, and toenail fungus.
Also known as tinea pedis, athlete’s foot is a common skin fungal infection of the foot. The fungi associated with this condition grow in warm, damp places and live on dead tissue surrounding the toenails, hair, and outer layers of the skin.
There are three different types of athlete’s foot. Interdigital athlete’s foot is the most common form, occurring between the smallest two toes and occasionally spreading to the sole. Moccasin athlete’s foot begins on the sole and spreads to the side of the foot. Vesicular athlete’s foot is the least common type and presents itself as blisters on the bottom of the foot.
How fungal skin infections develop
Fungi thrive in warm, moist environments. When the conditions are right, they can multiply on your skin, hair, or nails, leading to an infection. Minor cuts, scrapes, or breaks in the skin can make it easier for fungi to invade and grow.
Types of fungal infections
At Advanced Dermatology, P.C., our board-certified dermatologists provide compassionate, expert care for all types of fungal skin infections, ensuring effective treatment and comfort for every patient.
Ringworm (Tinea corporis)
Ringworm is a contagious skin infection that causes a red, circular, and itchy rash. According to data from the World Health Organization, ringworm accounts for half of all global fungal skin infections.
Despite its name, it is not caused by a worm. Instead, it is caused by a group of fungi called dermatophytes. Ringworm can appear on various parts of the body and is easily spread by skin-to-skin contact or by sharing personal items.
Tinea versicolor
Tinea versicolor causes small, discolored patches on the skin, usually on the upper body. These patches may be lighter or darker than the surrounding skin and may be mildly itchy.
Tinea versicolor is less contagious than ringworm and is often triggered by factors such as hot weather or sweating.
Toenail fungus (Onychomycosis)
Toenail fungus is a common infection that causes toenails to become thick, yellow, and brittle. It can also spread to fingernails. Toenail fungus grows slowly and can be difficult to treat, often requiring long-term therapy.
Dermatophyte and superficial fungal infections
Dermatophytes are a group of fungi that cause most skin, hair, and nail infections. Superficial fungal infections affect the outer layers of the skin and are usually not serious but can be uncomfortable and persistent.
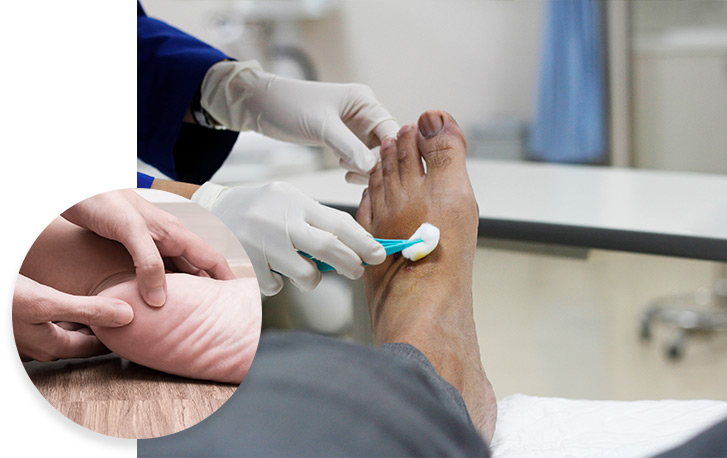
What is ringworm (Tinea corporis)?
Ringworm, also known as tinea corporis, is a fungal skin infection. While this condition is most common in children, it can affect people of all ages, including pets.
Ringworm grows in warm, moist areas such as swimming pools and locker rooms. Individuals typically catch ringworm through contact with people, pets, or items contaminated with the fungus. Ringworm can appear anywhere on the body.
Athlete’s foot
Treatment for athlete’s foot varies depending on the severity of the condition. Regardless of the severity, the feet must stay clean and dry to prevent the growth of additional fungi. Mild cases of athlete’s foot are often treated with topical medications, while oral medications may be necessary for more severe cases.
Ringworm
Most cases of ringworm can be treated with over-the-counter creams. Persistent cases may require prescription pills to clear the infection. Patients being treated for ringworm can continue their day-to-day activities without limitations. The exact course of treatment depends on each patient’s individual condition and medical history.
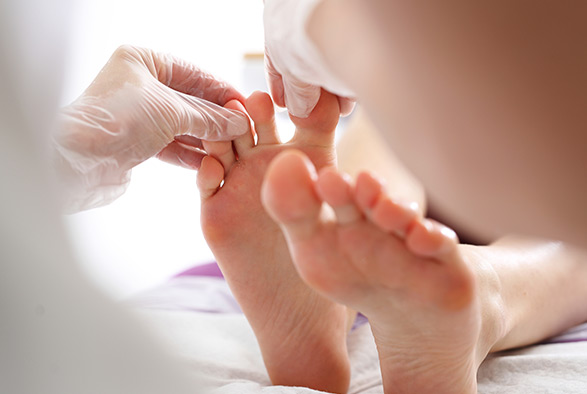
Causes of fungal skin infections
Fungal infections are caused by direct contact with fungi. Factors like warm, humid environments, sweating, wearing tight clothing, and poor hygiene can increase your risk. Sharing towels, shoes, or clothing with someone who has a fungal infection can also spread the fungi.
How do you get fungal infections?
You can get a fungal infection by coming into contact with contaminated surfaces, people, or animals. Walking barefoot in communal areas like locker rooms, sharing personal items, or having a weakened immune system can increase your risk of developing a fungal infection.
Are fungal infections contagious?
Many fungal infections, such as ringworm, are contagious. They can spread through direct skin-to-skin contact or by touching contaminated objects. Other fungal infections, like tinea versicolor, are less likely to spread between people.

Common symptoms of fungal infections by condition
Althete’s Foot
Symptoms of athlete’s foot include itching, burning, peeling, redness, blistering, or cracking of the skin on the feet. Patients experiencing these symptoms should contact their dermatologist to ensure proper care.
Ringworm
Ringworm typically causes a red, itchy rash. Despite its name, ringworm does not always present itself as rings. If you think you have signs of a rash, contact your dermatologist.
Symptoms of fungal infections on the skin and nails
Symptoms can vary but often include:
- Red, scaly, or itchy skin
- Circular or ring-shaped rash (ringworm)
- Discolored, thickened, or brittle nails (toenail fungus)
- White or yellowish patches on the skin (tinea versicolor)
If you notice these symptoms, it’s important to seek treatment to prevent the infection from spreading.
Diagnosing fungal infections
Athlete’s Foot
To diagnose athlete’s foot, your dermatologist will take a scraping of skin from the affected area and examine it under a microscope. This will determine whether a fungal infection is causing your symptoms.
Ringworm
To diagnose ringworm, your dermatologist will take a scraping of the rash and examine it under a microscope. This will determine whether ringworm is causing your red, itchy skin.
How dermatologists diagnose fungal infections
Dermatologists diagnose fungal infections by examining the affected area. They may scrape a small sample of skin or nail to look at under a microscope or send it to a lab for testing. This helps confirm the diagnosis and choose the best treatment.
Fungal Infection Treatment Options
Advanced Dermatology, P.C. offers effective treatment for all types of fungal skin infections, helping patients achieve healthy skin and nails through personalized care.
Ringworm treatment approaches
Mild cases of ringworm can often be treated with over-the-counter antifungal creams. For widespread or stubborn infections, prescription creams or oral antifungal medications may be needed.
Tinea versicolor treatment options
Tinea versicolor is usually treated with topical antifungal creams, lotions, or shampoos. In some cases, oral antifungal medications are prescribed if the infection is extensive or recurs frequently.
Toenail fungus treatment strategies
Toenail fungus is harder to treat and often requires oral antifungal medications taken for several months. Topical treatments can also help, but they are most effective for mild infections. In some cases, removing the affected nail may be necessary.
Antifungal treatment for skin
Most skin fungal infections respond well to antifungal creams, gels, or sprays. These are applied directly to the affected area for several weeks.
Oral antifungal medication for severe infections
For severe or persistent infections, oral antifungal drugs may be necessary. These medications are taken by mouth and work throughout the body to clear the infection.
How to treat fungal infections effectively
Follow your doctor’s treatment plan as directed. Finish the full course of medication, even if symptoms improve. Keeping the affected area clean and dry helps speed up recovery and prevents recurrence.

Fungal infection prevention
Athlete’s Foot
- Wear footwear in public locker or shower areas.
- Wash your feet daily.
- Dry your feet thoroughly after showering.
- Wear shoes that let your feet breathe.
Ringworm
- Dry your body completely after bathing or showering, making sure you dry your feet last.
- Wear adequate footwear in public shower and locker areas.
- Change socks and underwear daily.
- Refrain from sharing towels, sheets or clothing with others.
Everyday tips to prevent skin fungal infections
- Keep skin clean and dry.
- Change socks and underwear daily.
- Avoid sharing personal items.
- Wear sandals in communal showers or locker rooms.
- Choose breathable clothing and shoes.
- Treat any cuts or scrapes promptly.
When to see a dermatologist for a fungal infection
See a dermatologist if your infection does not improve with over-the-counter treatments, keeps coming back, or spreads rapidly. People with weakened immune systems should seek care promptly.
Signs you need a fungal infection specialist
- Severe pain, swelling, or pus
- Rapidly spreading rash
- Nail infections that don’t improve
- Repeated or long-lasting infections
Benefits of early treatment
Early treatment prevents the infection from spreading and helps avoid complications. It can also reduce discomfort and improve the appearance of your skin and nails.
Advanced Dermatology, P.C., fungal infection care
Our team provides expert evaluation and personalizes your treatment plan for the best results. We use the latest diagnostic techniques and medications to address your specific needs.
Please contact our caring team to discuss scheduling an evaluation and to answer any questions you might have regarding insurance coverage or payment plans.
Comprehensive care at our dermatology clinic for fungal infections
We offer a wide range of treatments for skin and nail fungal infections, from topical therapies to advanced oral medications. Our clinic supports you every step of the way, from diagnosis to follow-up care.
Frequently Asked Questions
How can I get athlete’s foot (tinea pedis)?
Athlete’s foot (tinea pedis) is caused by different fungi, including species of trichophyton, epidermophyton, and microsporum. You can get athlete’s foot when you come in contact with these fungi in a public shower, swimming pool, gym, or any other place where you go barefoot. Using slippers or other ventilating footwear is recommended to prevent athlete’s foot. In addition, it is recommended to refrain from sharing towels or socks with someone else. Furthermore, make sure you wash your towels and socks at a high temperature.
Why do I get athlete’s foot (tinea pedis)?
Fungi grow, multiply and contaminate the skin under conditions that are favorable to them.
There are 4 factors that can contribute to getting athlete’s foot:
- Moisture: Fungi can live and multiply on sweaty, warm, wet feet. Dry and ventilate your feet well.
- Poor hygiene: Dead skin tissue is like food to fungi. Wash your feet and change your socks frequently.
- Increased pH value: Where skin touches (between toes), the pH value of the skin increases. This may harm the barrier function of the skin. Make sure your shoes are not too tight and that you ventilate them often.
- Damaged skin: fungi may enter cuts or scratches. Using too much soap can harm the protective fatty acids that protect your skin. Rinse your feet well with water and dry thoroughly.
I like to do sports. Am I at risk of getting athlete’s foot (tinea pedis)?
The fungal infection of the foot, tinea pedis, is also called athlete’s foot. This term is used because it affects people with sweaty, damp feet, a condition common among athletes. However, engaging in sports does not necessarily increase the risk of athlete’s foot. Anyone can get athlete’s foot (tinea pedis), and you can prevent it by taking the right precautions.
When should I see a doctor for athlete’s foot (tinea pedis)?
Athlete’s foot usually starts between the toes or at the bottom of your feet. It gives an itchy, burning feeling, and the skin may look red and blistered, and might crack open.
As with all conditions, the right time to see a doctor for athlete’s foot is when you first notice symptoms. At an early stage, it may be treated with a topical cream; however, at a more advanced stage, oral medication could be more effective. A specialized dermatologist can recommend the most effective treatment for your case.
Is ringworm contagious to family members?
Yes, ringworm can easily spread between family members through direct contact or by sharing towels, bedding, or clothing.
Can fungal infections go away without treatment?
Some mild fungal infections may clear up on their own, but most require treatment to resolve and prevent spreading fully.
Why does toenail fungus take longer to treat?
Toenail fungus is difficult to treat because the infection is under the nail, which grows slowly. Medications may take several months to reach and clear the infection.
Can children get fungal skin infections?
Yes, children can get fungal skin infections, especially ringworm. Prompt treatment helps prevent spreading to others.
If you’re experiencing symptoms of a fungal skin or nail infection, contact the Advanced Dermatology, P.C. clinic near you to schedule expert care and effective treatment options.
